Treatment of corneal diseases
Dr. Marco Lombardo and his staff offer professional advice, diagnosis and treatment of corneal diseases. Below you will find the latest surgical techniques for the treatment of corneal diseases.
For more information or to book a visit, contact our staff.
Phototherapeutic keratectomy
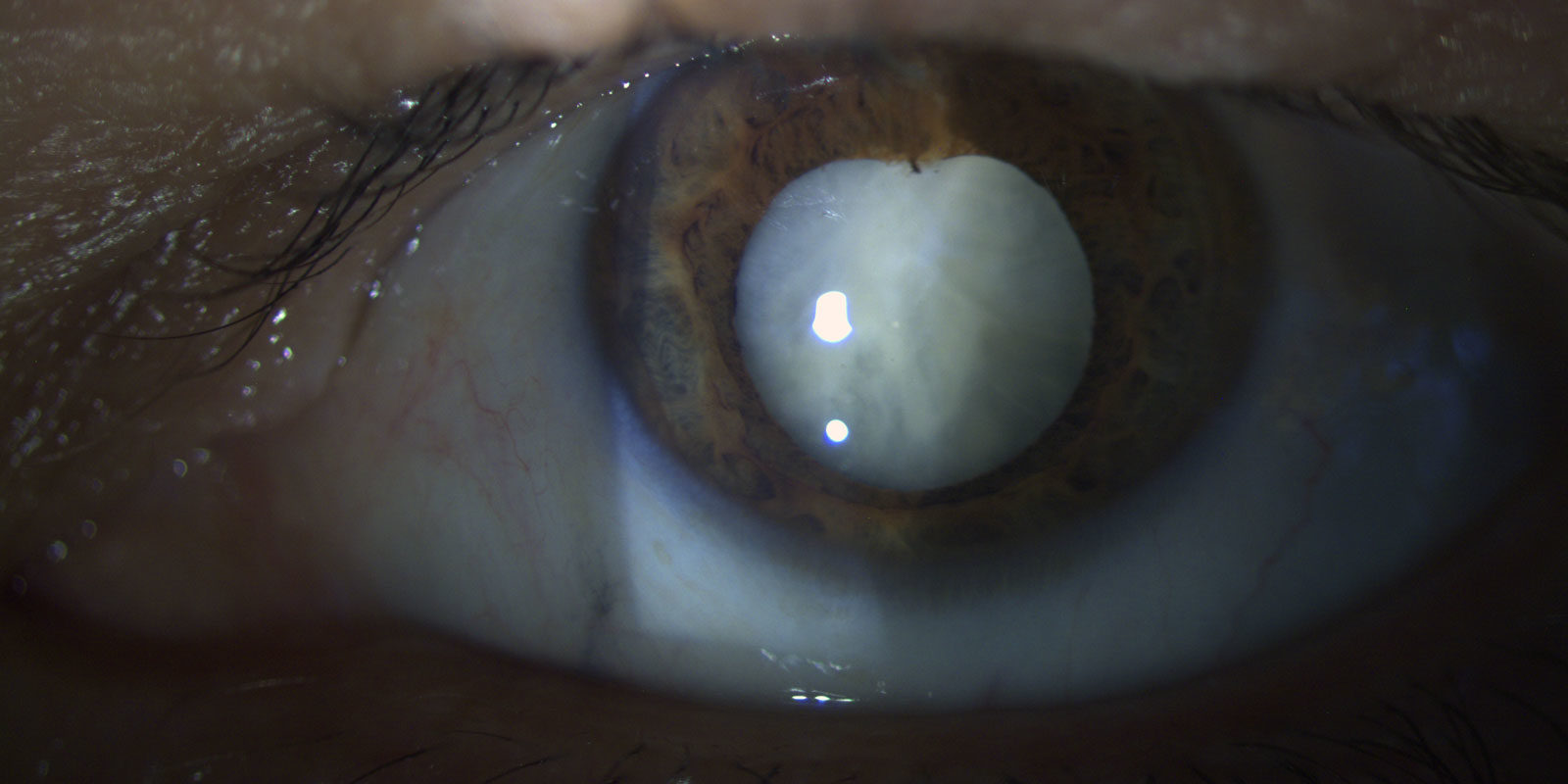
PTK or phototherapeutic keratectomy is a technique that is used to remove diseased corneal tissue and restore tissue transparency and regularity. It is used to remove anterior corneal scars caused by trauma, infections, corneal dystrophies.
Corneal transplantation
Corneal transplantation, or keratoplasty, is a surgical procedure aiming at replacing the diseased cornea with an eye bank donor cornea. There are various corneal transplantation techniques that vary depending on whether the pathology compromises the corneal tissue entirely or partially.
- Penetrating keratoplasty
Penetrating, or full-thickness, keratoplasty is still the most widespread technique of keratoplasty. It consists in replacing a full-thickness central portion of the damaged cornea with a transparent and healthy donor cornea. The donor tissue is sutured to the peripheral corneal host. Visual recovery is generally slow and requires months. The results achieved with the perforating keratoplasty in terms of visual acuity can be excellent, however a high astigmatism is common and may require additional treatments. The risk of transplant rejection is always present. - Deep anterior lamellar keratoplasty
Deep anterior lamellar keratoplasty consists of replacing the anterior portion of the corneal tissue. Surgical indications are keratoconus and anterior corneal scars caused by trauma or infection. The advantage of deep anterior lamellar keratoplasty with respect to penetrating keratoplasty is that it does not require full-thickness corneal removal. Complications are therefore less frequent than penetrating keratoplasty. - Endothelial keratoplasty
Endothelial keratoplasty consists of replacing the corneal endothelium; the most used techniques are termed DSAEK and DMEK. The indication for endothelial keratoplasty is Fuchs dystrophy or bullous keratopathy. Both are diseases that primarily affect the endothelium and may lead to the decompensation of the entire corneal tissue. The advantages of endothelial keratoplasty with respect to penetrating keratoplasty are numerous and include: visual recovery is more rapid, generally after one to three months from surgery the patient has an almost complete visual recovery and the intervention does not require sutures. The risk of rejection of the transplanted flap is also lower.
Stem cell transplantation
The corneal surface is covered by a layer of epithelial cells, the epithelium, which is maintained and constantly renewed by the action of the stem cells present at its edges (the corneal limbus). When corneal stem cells are damaged by chemicals, trauma, infection, contact lens abuse, a severe eye damage can occur leading to corneal opacification. In these cases, corneal transplantation alone is not enough to restore vision. It is therefore necessary before the transplant to reconstruct the corneal surface, through an autologous stem cell graft. The stem cells are taken from the patient’s healthy fellow eye and cultivated in the laboratory. At the end of the culture phase (about 3 weeks), the graft is placed onto the diseased eye.