Simulated vision in a case of advanced macular degeneration. A central dark spot reduces visual ability.
Macular diseases
Dr. Marco Lombardo and his staff offer professional advice, diagnosis and treatment of age-related macular degeneration and other macular diseases. The macula is the central area of the retina dedicated for improved vision. Any pathology affecting this area is referred to as macular disease.
At Studio Italiano di Oftalmologia of Dr. Marco Lombardo, the accurate diagnosis of macular disease is established in order to define the most appropriate therapy for each patient.
Age-related macular degeneration
Age-related macular degeneration , also known as AMD, is the most common cause of legal blindness in the Western world over 60 years.
There are two clinical forms of age-related macular degeneration, which are atrophic and exudative forms.
Aging is the most important risk factor ofage-related macular degeneration. It is recommended for patients to avoid smoking, to take a healthy lifestyle and to wear sunglasses with UV protection.
Diagnosis
The early stages of age-related macular degeneration are absolutely asymptomatic (without visual disturbances). Disease progression is accompanied by the appearance of more or less severe visual symptoms, such as “metamorphopsias” (vision of distorted images) and vision loss. In the atrophic AMD form, visual loss is gradual; it can be more rapid in the exudative AMD form.
The diagnosis of age-related macular degeneration is clinical, performed by fundus examination. Some diagnostic tests may be useful for determining the type of macular degeneration, including the Amsler grid, optical coherence tomography (OCT) and electroretinogram(mfERG).
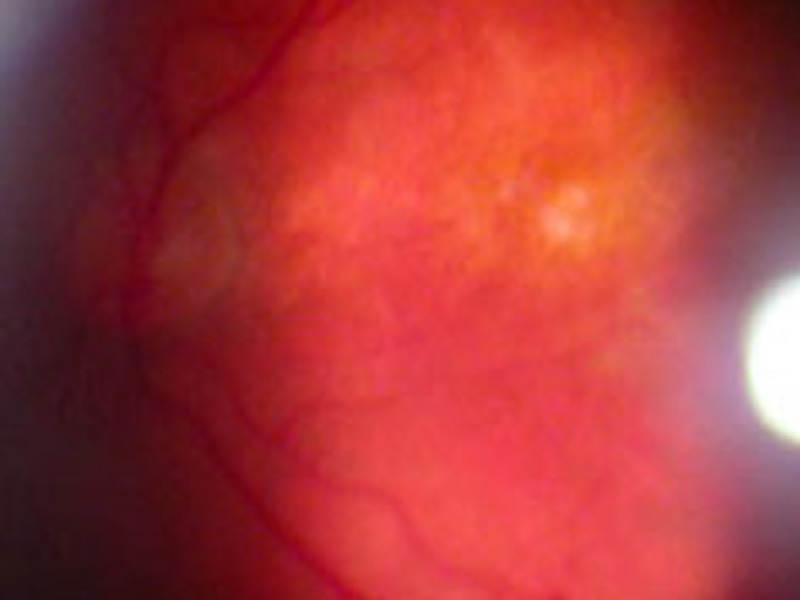
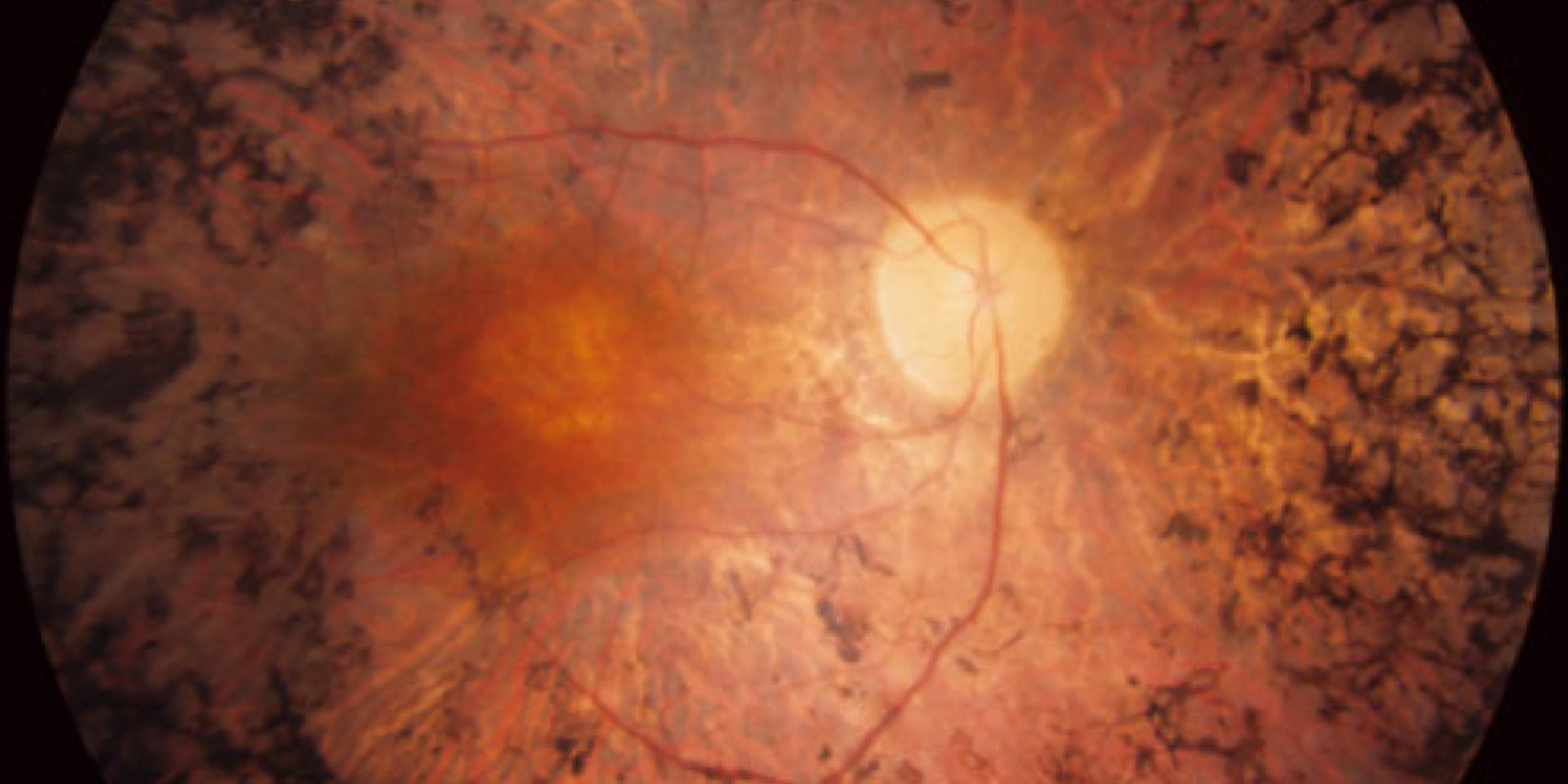
Atrophic AMD form
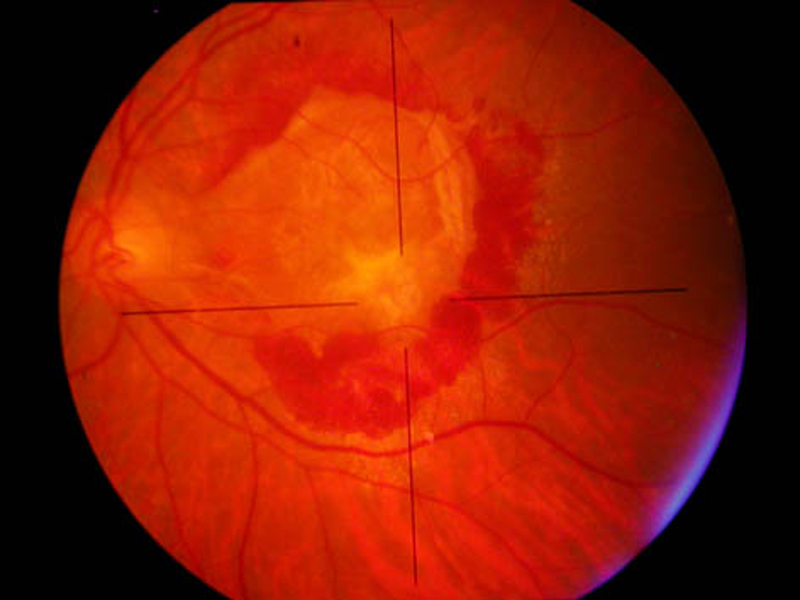
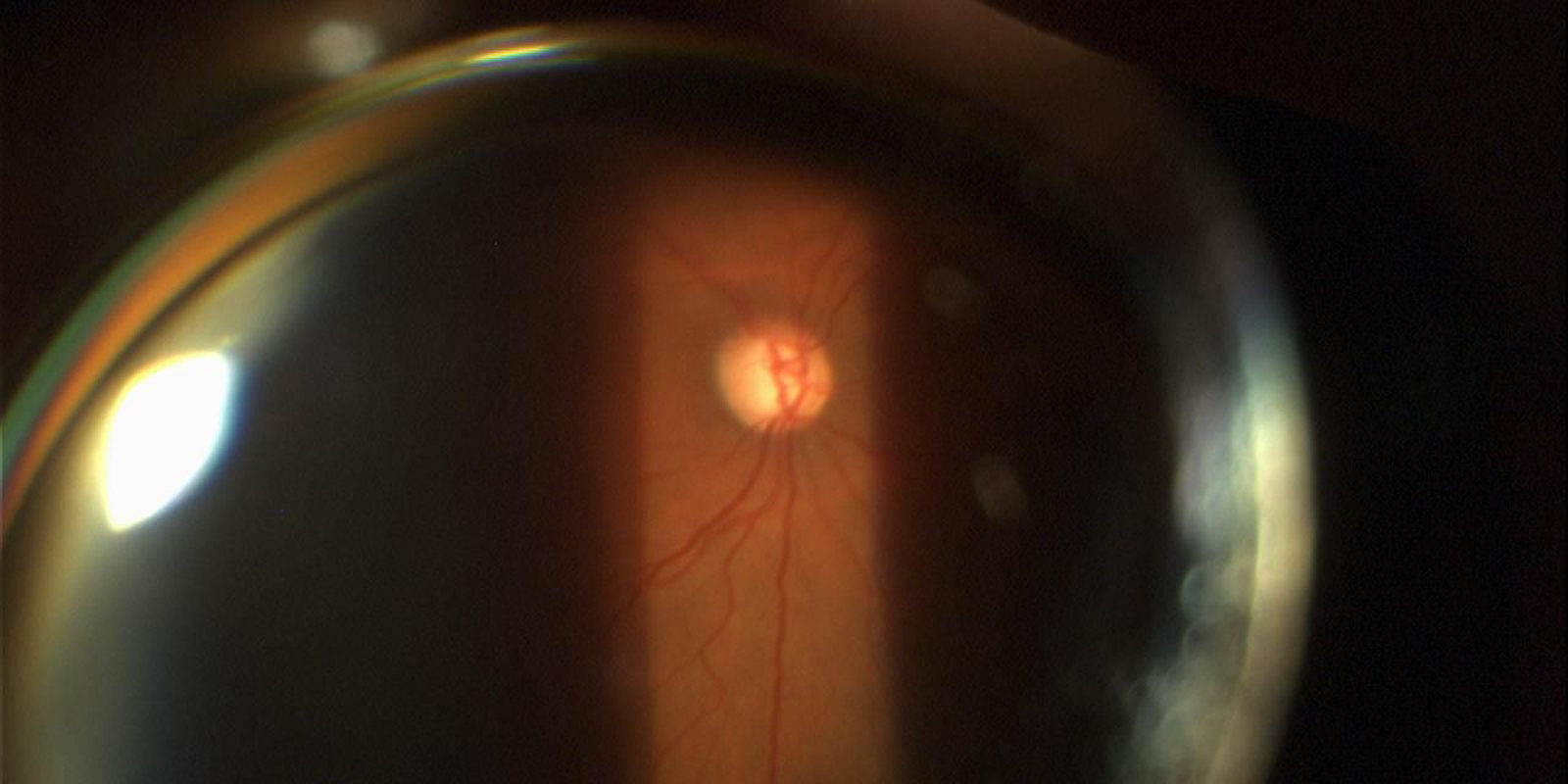
Exudative AMD form
Treatment of age-related macular degeneration
The Age-related Eye Disease Studies (AREDS) have shown that nutritional factors can prevent or reduce the incidence of the disease. Macular degeneration therapy involves the integration into the diet of lutein and zeaxanthin.
In the event that macular degeneration evolves towards the exudative form, it is necessary to intervene quickly to avoid serious complications. Three surgical options are available: photocoagulation treatment, photodynamic therapy and, more frequently, intravitreal injections of anti-angiogenic drugs.
- Intravitreal injections
Anti-angiogenics (anti-VEGF) are the most commonly used intravitreal drugs. There several anti-VEGF drugs available for macular degeneration, each of which may offer the chance of taking advantage of the greater positive effect of combined treatments (such as with photodynamic therapy). The anti-VEGF injections have been shown to be effective, in selected cases, in slowing down the progression of the sub-foveal neovascular membranes. - Photodynamic therapy
Photodynamic therapy consists of the intravenous administration of a photosensitizing drug, which is activated by the absorption of a red light projected onto the retina. The photosensitizing agent used for photodynamic therapy is verteporfin, which is a molecule that is selectively captured by newly formed capillaries; the luminous activation of the drug gives rise to a process that aim at occluding the neovessels. Photodynamic therapy is currently performed in combination with intravitreal injections. It still remains the primary choice in some patients, such as the treatment of myopic macular degeneration and chronic central serous chorioretinopathy. - Laser photocoagulation
Laser photocoagulation is indicated for the treatment of extrafoveal neovascular membranes. The procedure has as complications the formation of small scotomas (dark areas) in correspondence of the treated area or, in very rare cases, a reduction of the sight.